Movement Disorders Ecosystem
what sets us apart
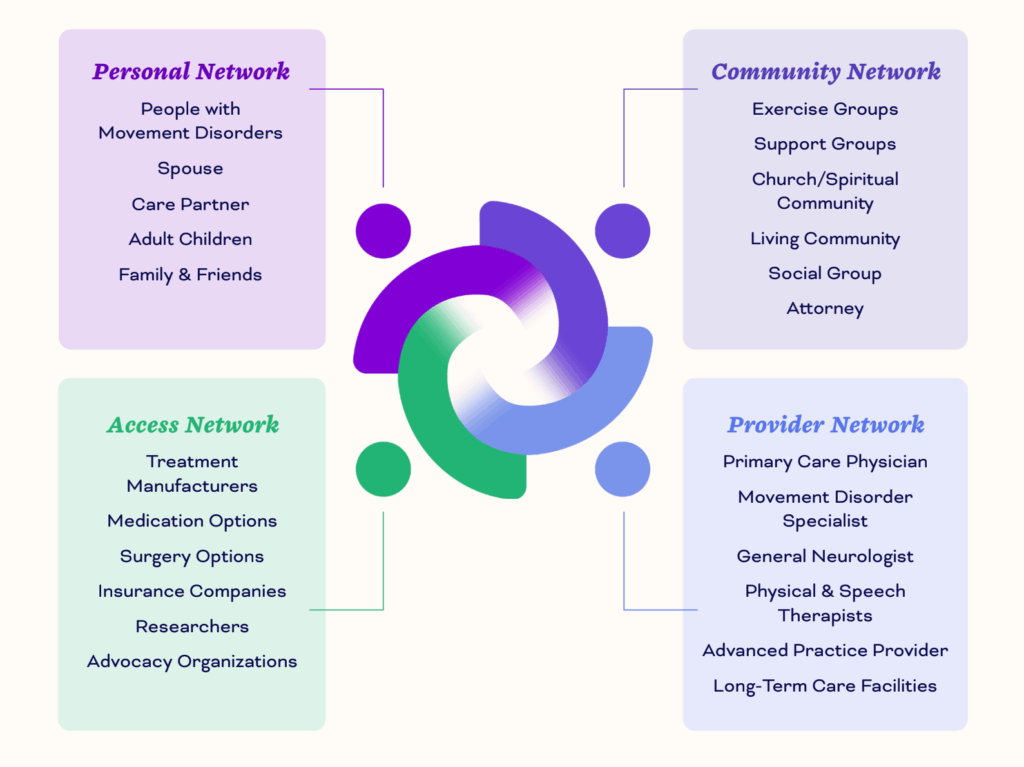
The Ecosystem
Our support doesn’t end with the person with a diagnosis, and it never did.
Our newly updated Movement Disorders Ecosystem embraces and serves everyone impacted by movement disorders—including those with lived experience, their community members, and their treatment providers—because quality-of-life is a collective pursuit, and we only reach the summit when we climb together.
Whatever your perspective, there’s a place for you here.
Click to learn about the
Personal Network
This network encompasses those who have personal, lived experience with a movement disorder.
Click to learn about the
Community Network
This network encompasses those who organize and educate their communities around movement disorders.
Click to learn about the
Provider Network
This network encompasses those with specialized training to provide services to improve quality-of-life.
Click to learn about the
Access Network
This network encompasses those who ensure treatments are safe, effective, and accessible.
Diagnosed & At-Risk • Care Partners • Family & Friends

Personal Network

The Personal Network includes:
- People with Movement Disorders
- Care Partner
- Adult Children
- Relatives
- Other Family & Friends
Group Leaders • Community Organizations • Advocates

Community Network

The Community Network includes:
- Exercise Groups
- Support Groups
- Financial Support & Resources
- Church/Spiritual Community
- Advocacy Organizations
- Living Community
- Social Group
- Attorneys
Healthcare • Therapy • Long-term Care

Provider Network

The Provider Network includes:
- Primary Care Physicians
- Movement Disorder Specialists
- General Neurologists
- Advanced Practice Providers
- Physical Therapists
- Speech Therapists
- Social Workers
- Long-Term Care Facilities
- & More!
Treatment Manufacturers • Insurance Companies • Researchers

Access Network

The Access Network includes:
- Treatment Manufacturers
- Medication & Surgery Options
- Insurance Companies
- Researchers
- Advocacy Councils
- Access Organizations

build your own ecosystem
Networks of Support
Now that you know our Ecosystem, it’s time to create your own!
Using our Movement Disorders Ecosystem framework, this resource was created so you can list everyone in your ecosystem! Not sure who to add? No problem: every member of every network is already listed for you.